“Bulged discs?”
Here’s what you need to know:
Two parts make up our spinal discs. One is the annulus which is the tough, hard outer shell. The other is the nucleus pulposus which is the inner gel like substance. Sometimes, the nucleus pulposus can protrude, or herniate, through the annulus, causing the disc to bulge and appear as if it has moved out of alignment with the spine. 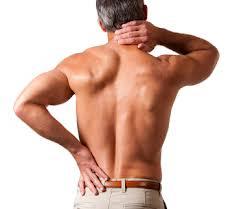
Prolapse: Where the disc bulges out between vertebrae although its hard outer layer is still intact.
When you have a prolapsed disc, a disc does not actually slip. What happens is that part of the inner softer part of the disc (the nucleus pulposus) bulges out (herniates) through a weakness in the outer part of the disc.
The bulging disc may press on nearby structures such as a nerve coming from the spinal cord. Some inflammation also develops around the prolapsed part of the disc.
Any disc in the spine can prolapse. However, most prolapsed discs occur in the lumbar part of the spine (lower back). The size of the prolapse can vary. As a rule, the larger the prolapse, the more severe the symptoms are likely to be.
How do discs bulge?
For most patients, disc herniation occurs as a normal part of the ageing process – the spine works very hard and sustains a good deal of wear and tear. As we get older, spinal discs lose some of their elasticity which leaves them more prone to cracking.
Occasionally, injury to the spine or traumatic events (such as falling, repetitive activities or heavy lifting) can lead to herniation too. Sneezing, awkward bending, or heavy lifting in an awkward position may cause some extra pressure on the disc. In people with a weakness in a disc, this may be sufficient to cause a prolapse.
Factors that may increase the risk of developing a prolapsed disc include: a job involving lots of lifting, a job involving lots of sitting (especially driving), weight-bearing sports (weight lifting, etc), smoking, obesity, and increasing age (a disc is more likely to develop a weakness with increasing age).
Contributing factors: poor core stability, a sedentary lifestyle, being overweight, muscle tightness, muscle weakness, joint stiffness, poor lifting technique, poor posture, a lifestyle involving large amounts of sitting, bending or lifting.
Symptoms of Bulged Discs
Herniated discs can cause compression on the nerves that run through the spinal column and this can be extremely painful. One of the most common symptoms of disc herniation in the lower part of the spine is ‘sciatica‘.
Other symptoms can include pain, numbness, tingling and burning sensations. These symptoms can appear on one or both sides of the body, extending down the arms and the legs. Pain caused by herniated discs is often worse at night, or after extended periods of sitting or standing.
One of the most bizarre things about herniated discs is that they can also be completely symptom free. They are often discovered during scans or surgery for other issues.
Back pain: The pain is often severe, and usually comes on suddenly. The pain is usually eased by lying down flat, and is often made worse if you move your back, cough, or sneeze.
Nerve root pain: Nerve root pain is pain that occurs because a nerve coming from the spinal cord is pressed on (trapped) by a prolapsed disc, or is irritated by the inflammation caused by the prolapsed disc. Although the problem is in the back, you feel pain along the course of the nerve in addition to back pain. Therefore, you may feel pain down a leg to the calf or foot. In the neck it can refer to the shoulder and arm. Nerve root pain can range from mild to severe, but it is often worse than the back pain
Other nerve root symptoms: The irritation or pressure on the nerve next to the spine may also cause pins and needles, numbness or weakness in part of a buttock, leg or foot. The exact site and type of symptoms depend on which nerve is affected.
How does Physiotherapy help with bulged discs?
Physiotherapy can be very effective in relieving the pain and other symptoms associated with herniated discs. Techniques such as neural gliding, joint mobilisation and dry needling are all known to be effective in treating this condition.
Your physiotherapist will also show you movements and positions to help relieve the pain and symptoms of disc herniation. Exercises to prevent further pain and damage also forms part of treatment.
In most cases, the symptoms tend to improve over a few weeks. Research studies of repeated MRI scans have shown that the bulging prolapsed portion of the disc tends to get smaller (regress) over time in most cases.
Continue with normal activities as far as possible. This may not be possible at first if the pain is very bad. However, move around as soon as possible, and get back into normal activities as soon as you are able. As a rule, don’t do anything that causes a lot of pain. However, you will have to accept some discomfort when you are trying to keep active.
This article gives a good overview of prolapsed discs and the use of painkillers in treatment.
Staying active during the acute stages is preferred over bed rest, as long as the activity does not aggravate the pain. This is why an early visit to your physiotherapist is critical in repairing the disc and relieving pain.
After Physiotherapy treatment:
Once healing begins to take place, we will tailor an exercise physiotherapy program that suits your needs and lifestyle. To promote good posture and restore normal function, core strengthening exercises should be done. Education in proper body mechanics such as lifting, bending, work habits etc. is vital in preventing a recurrence of the injury
Disc may be vulnerable to re-injury because of the factors that contribute to the original herniated discs. These include poor posture, lack of muscular stability, sporting and working habits that place large stresses on the discs. Therefore, the patient should follow the rehabilitation program set by the Physiotherapist to prevent re-injury. This will involve regaining the range of movement in the lumbar spine and strengthening the muscles which stabilise and support the back.
What to Learn More?
Interested to learn more about bulged discs? The physiotherapy Brisbane team from Pivotal Motion Physiotherapy can help answer all of your questions. Located in Newmarket, North Brisbane, call us on 07 3352 5116 or book an appointment online today!
Updated 12/03/2021