Easy Injury Prevention Tips: Achilles Tendon
The achilles tendon is the biggest tendon in the human body and injury to this tendon can be quite debilitating for most people. It’s no wonder that when referring to a person’s weak quality, people often use the term ‘achilles heel’.

The complexity in treating issues with achilles tendon can be overwhelming so we always advocate for prevention rather than treatment. This blog outlines what we believe are the best ways to avoid an achilles tendon injury. Before getting to this, here are some interesting facts on achilles tendon injuries:
- The incidence of achilles tendon ruptures in the general population is 5-10 per 100,000 but this is increasing overall.
- Competitive athletes have a lifetime incidence of achilles tendinopathy of 24 percent, with 18 percent sustained by athletes younger than 45 years.
- Achilles tendinopathy is common in runners. The incidence rate may be as high as 40-50%.
- The tendon gets weaker with age leading to increased risk of tendon rupture later in life.
- The risk factors for rupture are multi-factorial. This can include medical conditions such as autoimmune diseases, renal insufficiency and disorders of collagen; the type of activity you do (more common in runners).
- A normal tendon has a safety factor of 10. This refers to the strength and ability to withstand load. The higher a safety factor, the less chance of rupturing that tendon. The achilles tendon has a safety factor of 3.
The facts above demonstrate the need for better self-management. This leads into our tips. Here are our tips on what we believe is crucial to prevention of achilles injuries:
Improve Flexibility
The achilles is the tendon for the calf muscles which are the gastrocnemius (outer) and soleus (inner) muscles. Decreased flexibility in these muscles has been linked to increased risk for achilles tendon injuries. Poor flexibility particularly in the soleus muscle, leads to reduced shock absorption when running which leads eventually to achilles overload/injury. We recommend the following to help improve calf flexibility:
- Daily stretching – Stretching daily for 30-45 seconds and doing this a minimum of three times a day is great regime. The following photo shows how to stretch the gastrocnemius and soleus.
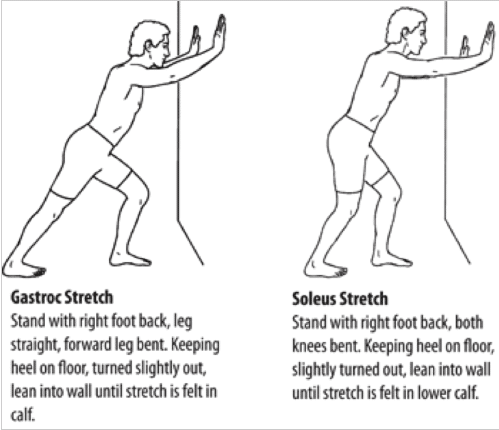
- Daily mobility – mobility is a very important factor for injury prevention. It involves putting the joint into positions to increase movement that the joint. To increase mobility, stand in a calf stretch position and bend the knee, you should feel a stretch in the back of the calf. Repeatedly bend and straighten the knee in this position. You should find that your mobility at the ankle increases.
- Self Trigger point releasing – Tight calves generally have many knots or ‘trigger points’knots or ‘trigger points’. A great way to relieve trigger points is to press the knotted areas of the muscle firmly on a ball or an object such as a foam roller and hold the pressure for a minute at a time.
- Heat – Applying heat to a muscle is a great way of increasing blood supply to the muscle promoting improved flexibility.
Pivotal Motion has massage balls, foam rollers, and heat packs available for purchase in the clinic.
Avoid Overload
This is very simple: when training for something, always gradually increase your training load to prevent overload. The key word here is gradually. It pays to write out a detailed training plan at the beginning, which outlines the weeks leading up to an activity or event. Sudden changes to training regimes such as changing terrain, drastically increasing distance or speed, decreasing rest periods, or changing footwear can cause unnecessary stress on the achilles which eventually leads to injury.
Check Your Footwear
Foot wear is a big factor because old, overworn shoes can cause overload on the achilles leading to injury. Overworn shoes tend to lose important properties such as shock absorption, which can increase the stress on the achilles with impact. It is recommended by physiotherapists to change footwear yearly especially shoes that are worn and used daily. We also recommend seeing a podiatrist to do a proper analysis of your foot biomechanics to determine the appropriate type of footwear.
Regular Calf Strengthening:
The achilles is the tendon the calf is directly attached to. Therefore, strengthening the calf leads to a stronger achilles tendon, which is less prone to injury.
Here are some nice calf exercises to help strengthen:
Standing Double Leg Calf Raise: Raise your heels from the ground so that you are standing on your tiptoes. Hold this for 5-10 seconds then slowly lower to the ground. You can progress this exercise to single leg and further increase it to a longer hold
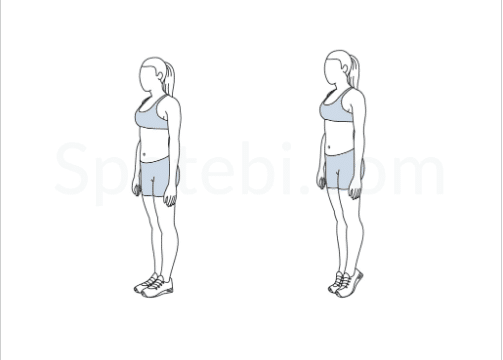
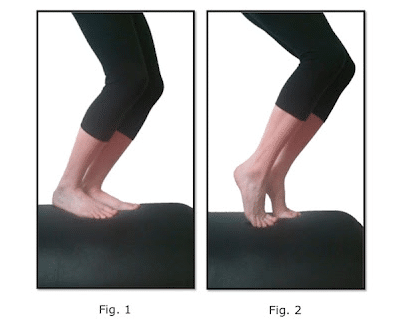
Standing Double Leg Calf Raise over a step: Raise your heels from a step so that you are standing on your tiptoes. Hold for 5-10 seconds then slowly lower past the step until you feel a stretch in the calf. Likewise in the first exercise, this exercise can be progressed to single leg and then by adding weight.
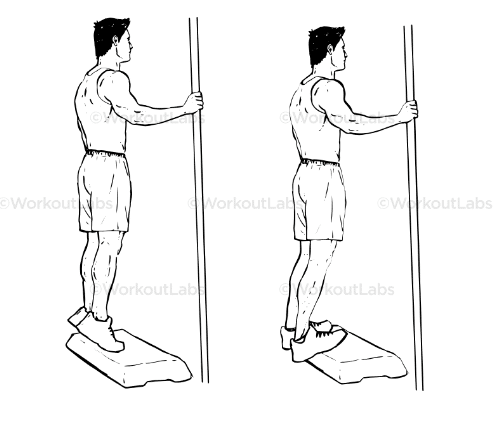
Bent Leg Double Leg Calf Raise: stand in front of wall/chair and hold for support. Bend the knees and flex your hips so that you’re nearly at 90 degrees of knee flexion. While keeping the knees bent, raise the heels from the ground until you are on your tiptoes. Hold this for 5-10 seconds then slowly lower to the ground.
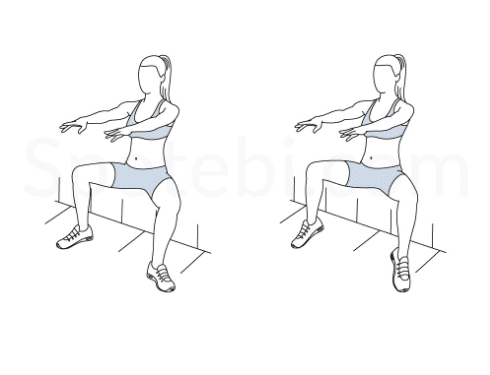
Calf Raise Wall Sit: Lay against a wall/sturdy surface and squat down so that your knees are 90 degrees. Raise your heels from the ground and stay on your tiptoes. Hold this position for 5-10 seconds then repeat.
These exercises can be progressed by adding light weights. For a proper calf-strengthening regime, it is best to come see us physiotherapists at Pivotal Motion.
Glute Strengthening
The gluteal muscles are at the top of the lower limb kinetic chain and they are essentially the powerhouse of the lower limb. This means that their strength greatly influences the stability and function of all the muscles and joints in the lower limb. The glutes are lateral rotators of femur, which means that when active, they pull the entire lower limb into the proper alignment which lessens the stress on the achilles. Here are common glute strengthening exercises that we highly recommend:
Glute Bridging: Start by lying on your back with knees bent and feet flat on the ground. Lift your bottom of the bed and squeeze your buttocks. Hold for 5 seconds before lowering. Repeat.

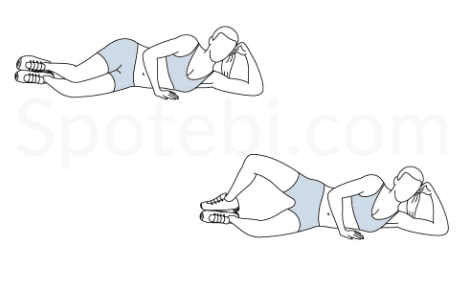
Clam Shells: Start in side lying with legs bent. Keeping the ankles together, lift your top knee from the bottom knee and squeeze through the buttocks. Hold for 5 seconds before lowering. Repeat.
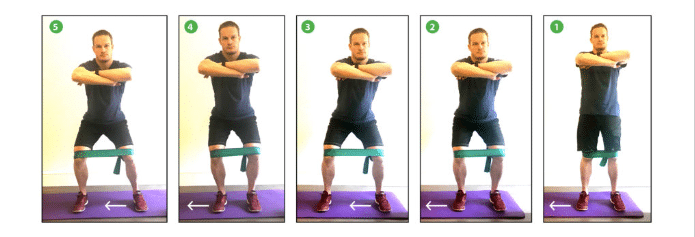
Crab Walking with resistance bands: Start by standing in a mini squat position with a theraband/resistance band around your knees. Step sideways towards one direction for 10 steps before stepping the opposite direction for also 10 steps. As you step out, you should feel the glutes contract.
These five tips are great ways to help with prevention of achilles injuries. For more information, or if you currently have an achilles injury, come and see our friendly team at Pivotal Motion Physiotherapy and Podiatry to help you out. Give us a call now or get in touch with us online to see how we can help you get the most out of your movement!