Jaw Pain & Injuries (TMJ)
When you visit us for physiotherapy for jaw pain, a jaw physiotherapist will do a thorough assessment of the function and mobility of your TMJ joint that will help determine if you might be suffering from TMJ disorder or other common jaw-related issues. If you’re searching for jaw physiotherapy, you have found the right place.
With years of treating patients suffering from a sore jaw joint, TMJ clicking, and other jaw-related issues, we help you by focusing on any underlying issues and providing the education, therapy, and rehabilitative exercises you need to get back on track.
Spesific conditions
Struggling with jaw pain?
At Pivotal Motion, physiotherapy for jaw pain is of special interest to our principle physiotherapist Bobbie-Jo Strong, and she will be eager to help with your recovery.
Call 07 3352 5116 to book a consultation or book online today.
WHAT WILL MY TMJ TREATMENT INVOLVE?
Jaw physiotherapy is important to ensure a proper and complete recovery from jaw pain. Though each injury will differ slightly, your jaw physio will guide you through the best treatment for your condition including:
- Education on jaw positioning, eating and chewing habits, and work or activity modification
- Heat or ice
- Postural correction
- Manual therapy
- Joint mobilisation – may involve manual techniques inside your mouth
- Rehabilitative exercises
- Referral to dentist or GP
We strive to educate our clients and patients on movement that is ideally suited to their individual needs. When you’re looking for ‘TMJ Physiotherapy near me’ contact a friendly and dedicated jaw physio from Pivotal Motion and let us help you with your sore jaw joint or TMJ pain today.
LEARN MORE ABOUT THE TEMPOROMANDIBULAR JOINT AND TMJ PAIN
The temporomandibular joint is the jaw joint. It is found just in front of and slightly below your earlobes on either side of your head. The two joints work together as a pair and connect the lower jawbone (mandible bone) to the temporal bones of the skull.
HOW DOES THE TMJ WORK?
HOW DOES THE TMJ WORK?
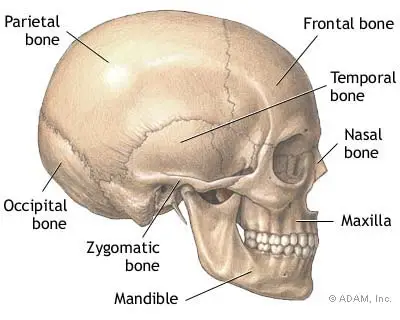
THE TMJ IS MADE UP OF:
- Mandible bone
- Temporal bone
- Zygomatic bone
- Disc
- Joint capsule
- Ligaments
- Muscles
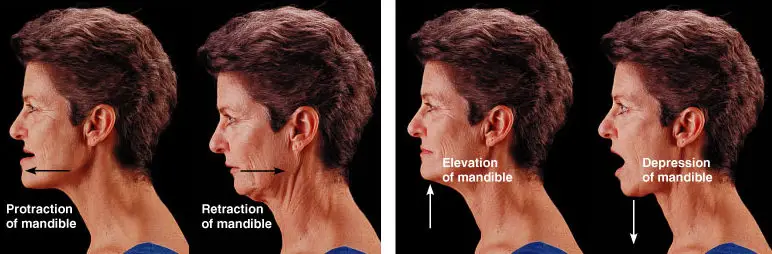
To keep the TMJ working smoothly, a soft disc lies between themandibular head and the articular fossa of the temporal bone. The disc also acts as a shock absorber when you chew. Normal movements of the mandible include opening (depression), closing (elevation), left, right, forward (protrusion), and backward (retrusion).
WHAT ARE TEMPOROMANDIBULAR DISORDERS?
WHAT ARE TEMPOROMANDIBULAR DISORDERS?
Temporomandibular disorders (TMD) and TMJ pain are injuries or issues that can affect any part of the TMJ. Also note, injuries or conditions that commonly affect other joints in the body such as arthritis, can also affect one or both of the TMJs.
Approximately 12% of the population have suffered from TMD associated jaw pain. Both men and women can experience TMD, but the majority are women aged 16-35 years.
The duration of TMDs can vary widely, with people experiencing symptoms anywhere from several days to several months.

SYMPTOMS OF TEMPOROMANDIBULAR DISORDERS (TMD)
Are you experiencing one or more of these symptoms and looking for a ‘TMJ Physio near me’? Then please contact us today to discuss using jaw physiotherapy to help treat your condition.
- Pain in the face, jaw, neck, or upper shoulders
- Headaches
- Ear pain, pressure, fullness, or ringing
- Jaw muscle stiffness, locking, or limited movement
- TMJ clicking or other noises, such as popping and grinding
- Changes to speaking, swallowing, breathing, and/or facial expressions
- Painful chewing
- A bite that feels ‘off’
- Dizziness
- Vision problems
- Swollen face or jaw
WHAT CAUSES TEMPOROMANDIBULAR DISORDERS?
Often there can be no cause for TMD symptoms, or there may be several contributing factors. Some possible causes of TMD include:
- The structure of the TMJ joint and it’s components
- Autoimmune diseases
- Trauma such as car accidents
- Stress
- Excessive use with gum chewing, nail-biting, smoking, singing
- Infections
- Dental procedures
- Prolonged mouth opening or jaw positions
- Arthritis
- Teeth clenching or grinding
What will my TMJ treatment involve?
Jaw physiotherapy is important to ensure a proper and complete recovery from jaw pain. Though each injury will differ slightly, your jaw physio will guide you through the best treatment for your condition including:
- Education on jaw positioning, eating and chewing habits, and work or activity modification
- Heat or ice
- Postural correction
- Manual therapy
- Joint mobilisation – may involve manual techniques inside your mouth
- Rehabilitative exercises
- Referral to dentist or GP
We strive to educate our clients and patients on movement that is ideally suited to their individual needs. When you’re looking for ‘TMJ Physiotherapy near me’ contact a friendly and dedicated jaw physio from Pivotal Motion and let us help you with your sore jaw joint or TMJ pain today.
Learn more about the Temporomandibular Joint and TMJ pain
The temporomandibular joint is the jaw joint. It is found just in front of and slightly below your earlobes on either side of your head. The two joints work together as a pair and connect the lower jawbone (mandible bone) to the temporal bones of the skull.
The TMJ is a complex structure that we use to eat, talk, and breathe. As one of the most used joints in the body, it is prone to an increased risk of jaw-related issues including:
- Sore jaw joint
- Intense jaw ache
- Sprained jaw
- A dislocated jaw
- A fractured jaw
How does the TMJ work?
The TMJ is made up of:
- Mandible bone
- Temporal bone
- Zygomatic bone
- Disc
- Joint capsule
- Ligaments
- Muscles
To keep the TMJ working smoothly, a soft disc lies between themandibular head and the articular fossa of the temporal bone. The disc also acts as a shock absorber when you chew. Normal movements of the mandible include opening (depression), closing (elevation), left, right, forward (protrusion), and backward (retrusion).

What are Temporomandibular Disorders?
Temporomandibular disorders (TMD) and TMJ pain are injuries or issues that can affect any part of the TMJ. Also note, injuries or conditions that commonly affect other joints in the body such as arthritis, can also affect one or both of the TMJs.
Approximately 12% of the population have suffered from TMD associated jaw pain. Both men and women can experience TMD, but the majority are women aged 16-35 years.
The duration of TMDs can vary widely, with people experiencing symptoms anywhere from several days to several months.


Symptoms of Temporomandibular Disorders (TMD)
Are you experiencing one or more of these symptoms and looking for a ‘TMJ Physio near me’? Then please contact us today to discuss using jaw physiotherapy to help treat your condition.
- Pain in the face, jaw, neck, or upper shoulders
- Headaches
- Ear pain, pressure, fullness, or ringing
- Jaw muscle stiffness, locking, or limited movement
- TMJ clicking or other noises, such as popping and grinding
- Changes to speaking, swallowing, breathing, and/or facial expressions
- Painful chewing
- A bite that feels ‘off’
- Dizziness
- Vision problems
- Swollen face or jaw
What causes Temporomandibular Disorders (TMD)?
Often there can be no cause for TMD symptoms, or there may be several contributing factors. Some possible causes of TMD include:
- The structure of the TMJ joint and it’s components
- Autoimmune diseases
- Trauma such as car accidents
- Stress
- Excessive use with gum chewing, nail-biting, smoking, singing
- Infections
- Dental procedures
- Prolonged mouth opening or jaw positions
- Arthritis
- Teeth clenching or grinding
Why do I have a sore jaw after dental surgery or dental work?
A sore jaw joint or some stiffness is common after oral surgery or prolonged dental work. This can last for several days or several weeks. This is often due to the prolonged mouth open position and if the surgery or dental work has affected structures surrounding the jaw.
Moderate to severe jaw pain, limited mouth opening, jaw locking, or TMJ clicking is not usually expected. This can be due to muscle strain or disc displacement associated with the prolonged mouth open position. In this case, you should seek advice from your dentist, doctor, and/or jaw physio.
Jaw physiotherapy can help alleviate the stiffness or soreness and help improve the amount of mouth opening you can achieve following surgery. Your jaw physio may advise using hot or cold therapy, regular jaw movement, and gentle jaw exercises.
Do I suffer from a different jaw-related issue?
While TMJ disorder is relatively common among both young and older adults, your jaw associated pain could be the symptom of other underlying issues including:
Jaw Dislocation
A jaw dislocation is when the joint dislocates sideways, upwards, forwards or backward, and cannot return to its normal position. Dislocations can be caused by dental treatments, intubation, trauma, arthritis, and even the wide opening of the mouth. Symptoms of a dislocated jaw include the inability to close/open your mouth, pain, difficulty speaking, drooling, and misalignment of the jaw, lips, and/or teeth.
Broken Jaw
A jaw fracture or broken jaw is when the jawbone is broken. This is often due to significant trauma which could be a direct blow, physical contact/assault, or motor vehicle accident. Jaw fractures can be small, where the bone is still in place, or large when the bones are significantly displaced. You might have a broken jaw if you are experiencing significant pain, swelling, difficulty with jaw movement, bleeding, or bruising.
Jaw Strain
A jaw strain is when the muscle fibres cannot cope with the demand that is placed on them. This is often due to a powerful muscle contraction or simply through repetitive use of the jaw. You might have a jaw sprain if you experience muscle stiffness, TMJ pain, tenderness, headaches, earaches, TMJ clicking, and more.
Who can help with TMJ treatment?
While TMJ disorder is relatively common among both young and older adults, your jaw associated pain could be the symptom of other underlying issues including:
Jaw Physiotherapist
physiotherapy for jaw pain can help by using different techniques to decrease jaw pain and improve the functioning of your jaw.
General Practitioner (GP)
many conditions can mimic the symptoms of TMD, so it is a good idea to get checked by your GP. Depending on the severity of your TMJ pain, they will also provide guidance on medications for pain management.
Dentist
they may prescribe a splint/guard to provide stabilisation or jaw repositioning. These are intended as short-term tools and are usually only used for a short period of time.
Struggling with jaw pain?
At Pivotal Motion, physiotherapy for jaw pain is of special interest to our principle physiotherapist Bobbie-Jo Strong, and she will be eager to help with your recovery.
Call 07 3352 5116 to book a consultation or book online today.
