What Are Sternoclavicular Joints?
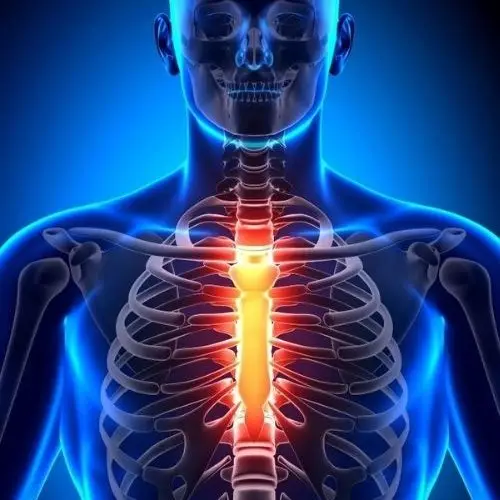
Sternoclavicular joints are where your collar bones meet the top of your breast bone called the manubrium (one on each side). This is quite a mobile joint, with only 50% of joint surface in contact at the same time, with discs and ligaments providing it with stability.
Studies have shown that your sternoclavicular joint can refer pain up into your neck and jaw, as well as along your collar bone towards your shoulder. Given that the heart can also refer into this area, the first thing that needs ruling out is a heart attack.
How can you injure the Sternoclavicular Joints?
Injuries to this area are associated with tenderness over the joint, sometimes with swelling and crepitus (noise coming from the joint when you move it). There will usually be pain with elevating your arm, bringing your shoulders forward, and reaching across your body.
Sternoclavicular joint injuries are quite rare. For example, the sternoclavicular joint only accounts for 1% of all shoulder dislocations. By far the most common cause of symptoms in this area is osteoarthritis, which occurs in older populations and manual labourers. Usually this will consist of 3-6 months of pain where a joint thickening will occur, and then the pain will dissipate.
Much less common conditions include can include:
- Subluxations (or partial dislocations) – these can occur after trauma, but are most often seen in young people with hypermobility.
- Condensing osteitis – swelling and sclerosis of the end of the collar bone closest to your breast bone. Most commonly occurs in younger women.
- Friedrich’s disease – spontaneous onset of pain in the sternoclavicular joint, can occur at any age but more common in children/adolescents. It’s been described as a self-limiting condition that usually resolves with conservative management.
- Various inflammatory conditions such as SAPHO, psoriatic arthritis, Tietze’s syndrome, costochondritis, infection, Reiter’s syndrome, gout and axial spondyloarthropathy.
How do you treat Sternoclavicular Joints injuries?
Sometimes your physiotherapist will request an x-ray as a first line screen due to the relatively infrequent presentations of musculoskeletal conditions in this area. Once deemed appropriate, treatment/rehabilitation will usually consist of:
- Advice and education on management.
- Muscle release techniques to settle down any secondary areas and potential contributing factors.
- Strengthening and stretching exercises for your shoulder, neck and chest.
- Supportive modalities eg. Taping, if indicated.
- Facilitate transition back to your usual activities

Sternoclavicular injury?
For the correct rehabilitation program for Sternoclavicular Joints Injuries, come see our experienced Physiotherapist at Pivotal Motion. Book an appointment online or call us today on 07 3352 5116.

